Contact Information
Research Interests
Cancer, Developmental Biology, Endocrinology, Epigenetics, Gene Regulation, Ion Channels
Research Description
Regulation of prostate development and growth by hormone receptor signaling pathways
The major goals of my research have been to understand how the prostate gland develops and how disruption of hormone receptor signaling pathways early in prostate development predisposes humans and rodents to neoplasia. Prostate neoplasia is a leading cause of urologic disease among men. Indeed, most lower urinary tract symptoms in men over age 50 are due to benign prostatic hyperplasia, and prostate cancer is the second leading cause of cancer-related deaths in men. Studies of genetically modified mice suggest that the androgen receptor (AR) plays a role in prostate neoplasia initiation. Androgens, like testosterone, and AR signaling are necessary for prostate development and homeostasis, and disruption of AR-mediated prostate development predisposes humans and rodents to prostate neoplasia by altering the gland’s phenotype early in life. Due to the involvement of AR in both prostate development and neoplasia, a thorough understanding of how AR controls cell proliferation and differentiation during prostate development will offer clues to key developmental events that reemerge in prostate neoplasia.
A fundamental question is how hormones, such as androgens and growth factors, regulate nearly all aspects of the development and growth of the prostate gland. Importantly, the AR does not act alone, rather it directs prostate development and neoplasia by molecular intersection, or crosstalk, with other signaling pathways. My laboratory utilizes an innovative organ culture system and complementary mouse models for prostate development and modern genomic and signaling pathway analyses to identify novel crosstalk between the AR and growth factor signaling pathways that control cell proliferation and differentiation to orchestrate prostate development and growth regulation.
My laboratory’s research is focused on the following biological problems:
- Identification of novel molecular players in prostate development. The prostate gland is formed from the embryonic urogenital sinus (UGS), where the urethra joins the bladder. Based on tissue recombination studies of UGS mesenchyme and epithelium from wild-type mice or mutant mice lacking functional AR, it has been suggested that AR action in the inductive mesenchyme controls the expression of morphogenetic genes, which act as paracrine factors to promote the proliferation of prostate progenitor cells and outgrowth of prostate epithelial (PrE) buds. In time, PrE progenitor cells must be directed to exit the cell cycle and differentiate into secretory luminal cells. Despite the importance of the AR as a hormone-activated transcriptional regulator in the male UGS and prostate, little is known of how the AR controls prostate development, and the nature of the AR-regulated morphogenetic genes is not understood. Thus, my laboratory has employed a functional genomics approach to identify novel androgen-responsive genes in the UGS and prostate of mice.
- AR-mediated growth suppression of PrE cells and proliferation of prostate cancer cells. The control of PrE cell proliferation is central to prostate development, homeostasis, and neoplasia. As PrE buds give rise to ducts in the developing prostate, PrE progenitor cells are directed to exit the cell cycle and differentiate into secretory luminal cells. AR signaling suppresses the proliferation and promotes the differentiation of luminal PrE cells. In contrast, AR activation stimulates the proliferation of prostate cancer cells. However, the mechanisms responsible for AR-mediated proliferation and differentiation of PrE cells are not well understood. In future studies, we expect to elucidate the nature of the “malignancy switch” that occurs as AR signaling switches from driving a differentiation program in normal PrE cells to a proliferation program in prostate cancer cells.
- AR-mediated regulation of the cellular stress response and apoptotic death of PrE cells. Proper tissue development and homeostasis require a balance of cell proliferation and a form of programmed cell death known as apoptosis, which removes excess unwanted cells and stressed damaged cells. In prostate neoplasia, the uncontrolled proliferation of neoplastic PrE cells without a compensatory increase in their apoptosis disrupts this balance. An ideal therapeutic regimen for malignant PrE cells would suppress their uncontrolled proliferation and promote their apoptosis. Thus, it is crucial to understand the mechanisms underlying the survival and death of PrE cells.
- Inhibition of AR activity. As the androgen receptor is a ligand-activated transcriptional regulator, drug development of AR antagonists has commonly focused on mechanisms that reduce hormone production or novel AR ligands. My collaborators and I have demonstrated that AR signaling can be inhibited in vivo by ligand-independent, non-competitive inhibitors, using the mouse prostate as a model. In future studies, we expect to identify the molecular targets of such inhibitors and define the roles of the molecular targets in AR signaling.
Education
B.S. 1995 University of Wisconsin, Eau Claire, WI
PhD. 2003 Johns Hopkins University-SOM, Baltimore, MD
Postdoc. University of California, San Francisco, CA
Additional Campus Affiliations
Associate Professor, Molecular and Integrative Physiology
External Links
Highlighted Publications
Representative Publications
Copeland BT, Pal SK, Bolton EC, and Jones JO. The androgen receptor malignancy shift in prostate cancer. Prostate. 2018 May; 78(7):521-531. PMID: 29473182.
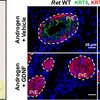
Park HJ and Bolton EC. RET-mediated glial cell line derived neurotrophic factor signaling inhibits mouse prostate development. Development. 2017; 144(12):2282-2293. PMID: 28506996.
Smith JW, Ford NA, Thomas-Ahner JM, Moran NE, Bolton EC, Wallig MA, Clinton SK, and Erdman JW. Mice lacking β-carotene-15,15’-dioxygenase (BCO1) exhibit reduced serum testosterone, prostatic androgen receptor signaling, & prostatic cellular proliferation. Am J Physiol Regul Integr Comp Physiol. 2016; 311(6):R1135-R1148. PMID: 27629887.
Chen C, Dienhart JA, and Bolton EC. Androgen-sensitized apoptosis of HPr-1AR human prostate epithelial cells. PLoS One. 2016; 11(5):e0156145. PMID: 27203692.
Kim YC, Chen C, and Bolton EC. Androgen receptor-mediated growth suppression of HPr-1AR and PC3-Lenti-AR prostate epithelial cells. PLoS One. 2015; 10(9):e0138286. PMID: 26372468.
Park HJ and Bolton EC. Glial cell line-derived neurotrophic factor induces cell proliferation in the mouse urogenital sinus. Mol Endocrinol. 2015; 29(2): 289-306. PMID: 25549043.
Zhou Y, Bolton EC, and Jones JO. Androgens and androgen receptor signaling in prostate tumorigenesis. J Mol Endocrinol. 2015; 54(1): R15-R29. PMID: 25351819.
Mukherjee S, Cruz-Rodriguez O, Bolton E, and Iñiguez-Lluhí JA. The in vivo role of androgen receptor SUMOylation as revealed by androgen insensitivity syndrome and prostate cancer mutations targeting the proline/glycine residues of synergy control motifs. J Biol Chem. 2012; 287(37): 31195-206. PMID: 22829593.
Jones JO, Bolton EC, Huang Y, Feau C, Guy RK, Yamamoto KR, Hann B, and Diamond MI. Non-competitive androgen receptor inhibition in vitro and in vivo. Proc Natl Acad Sci U S A. 2009; 106(17): 7233-7238. PMID: 19363158.
Bolton EC, So AY, Chaivorapol C, Haqq CM, Li H, and Yamamoto KR. Cell- and gene-specific regulation of primary target genes by the androgen receptor. Genes and Dev. 2007; 21(16): 2005-2017. PMID: 17699749.
So AY, Chaivorapol C, Bolton EC, Li H, and Yamamoto KR. Determinants of cell- and gene-specific transcriptional regulation by the glucocorticoid receptor. PLoS Genet.2007; 3(6): e94. PMID: 17559307.
Recent Publications
Kim, E. C., Zhang, J., Tang, A. Y., Bolton, E. C., Rhodes, J. S., Christian-Hinman, C. A., & Chung, H. J. (2021). Spontaneous seizure and memory loss in mice expressing an epileptic encephalopathy variant in the calmodulin-binding domain of Kv7.2. Proceedings of the National Academy of Sciences, 118(51), Article e2021265118. https://doi.org/10.1073/pnas.2021265118
Zhang, J., Kim, E. C., Chen, C., Procko, E., Pant, S., Lam, K., Patel, J., Choi, R., Hong, M., Joshi, D., Bolton, E., Tajkhorshid, E., & Chung, H. J. (2020). Identifying mutation hotspots reveals pathogenetic mechanisms of KCNQ2 epileptic encephalopathy. Scientific reports, 10(1), Article 4756. https://doi.org/10.1038/s41598-020-61697-6
Copeland, B. T., Pal, S. K., Bolton, E. C., & Jones, J. O. (2018). The androgen receptor malignancy shift in prostate cancer. Prostate, 78(7), 521-531. https://doi.org/10.1002/pros.23497
Park, H. J., & Bolton, E. C. (2017). RET-mediated glial cell line-derived neurotrophic factor signaling inhibits mouse prostate development. Development (Cambridge), 144(12), 2282-2293. https://doi.org/10.1242/dev.145086
Chen, C., Dienhart, J. A., & Bolton, E. C. (2016). Androgen-sensitized apoptosis of HPr-1AR human prostate epithelial cells. PloS one, 11(5), Article e0156145. https://doi.org/10.1371/journal.pone.0156145